If you’ve been diagnosed with diabetic retinopathy, you may be wondering what happens next. This condition affects the blood vessels in your retina and, over time, can interfere with your ability to see clearly.
Many patients feel anxious after hearing the diagnosis, but effective diabetic retinopathy treatment options exist to help protect your remaining vision. Understanding how your eye doctor approaches treatment, from early monitoring to advanced procedures, can help you feel more prepared and confident about your next steps.
What Is Diabetic Retinopathy?
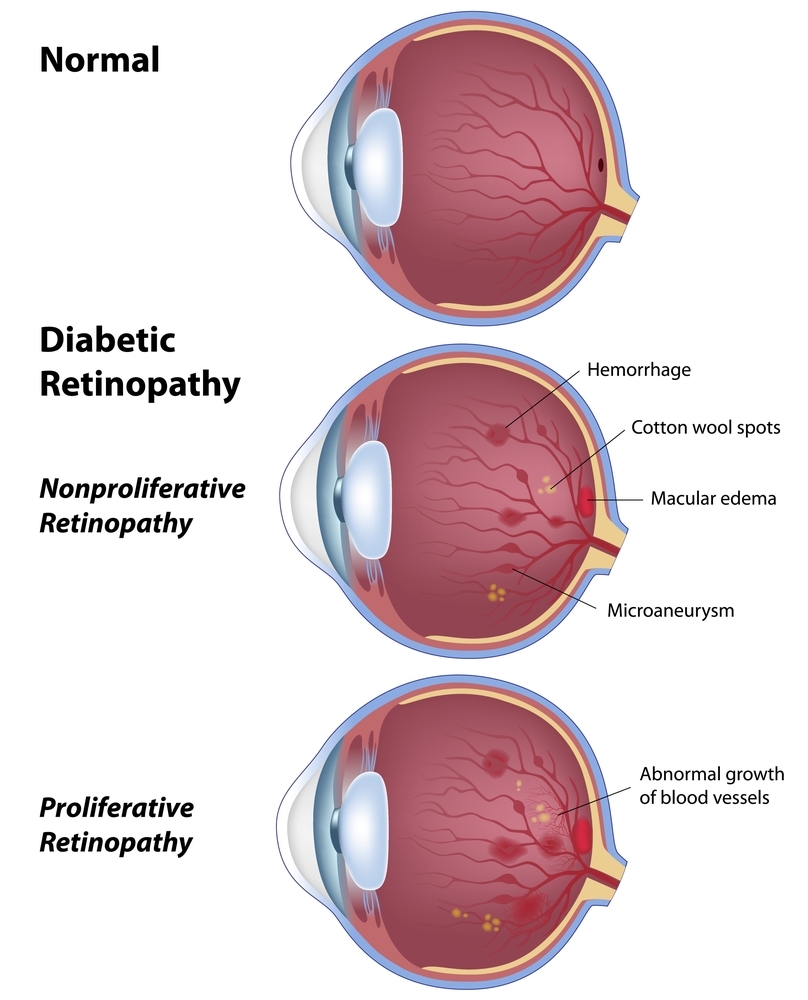
Diabetic retinopathy develops when consistently high blood sugar levels damage the small blood vessels that supply the retina, the light-sensitive layer of tissue at the back of your eye. Over time, these weakened vessels can swell, leak fluid, or completely close off. In some cases, the eye responds by forming new, fragile blood vessels prone to bleeding.
Eye doctors classify the condition into two main types. Nonproliferative diabetic retinopathy (NPDR) is the earlier, more common form. During this stage, the walls of the retinal blood vessels weaken and may develop small bulges that leak fluid or blood.
Proliferative diabetic retinopathy (PDR) is more advanced. In PDR, damaged blood vessels close off and trigger the growth of abnormal new vessels on the surface of the retina. These fragile vessels can bleed into the vitreous (the gel-like center of the eye), form scar tissue, and, in severe cases, lead to retinal detachment or glaucoma.
One challenge with this condition is that it often produces no noticeable symptoms in its early stages. By the time a patient notices floaters, blurred vision, or dark spots, the disease may have already progressed significantly.
How Is Diabetic Retinopathy Diagnosed?
The primary tool for detecting diabetic retinopathy is a dilated eye exam. During this exam, your eye doctor places drops in your eyes to widen the pupils, allowing a detailed view of the retina and the blood vessels inside the eye.
Your eye doctor may also use additional diagnostic tools. Optical coherence tomography (OCT) creates detailed cross-sectional images of the retina, showing whether fluid has leaked into the tissue.
Fluorescein angiography involves injecting a special dye into a vein in your arm and then photographing the retina as the dye circulates. This test helps identify blood vessels that are leaking, closed, or broken.
Because diabetic retinopathy can develop silently, the American Academy of Ophthalmology recommends that all patients with type 1 or type 2 diabetes have a comprehensive dilated eye exam at least once a year. Early detection gives you the best chance to preserve your vision.
How is Early-Stage Diabetic Retinopathy Treated?
If your eye doctor identifies mild or moderate nonproliferative diabetic retinopathy, you may not need immediate treatment. Instead, they will monitor your eyes closely with regular exams to track any changes in the retina and determine when to begin treatment if the condition worsens.
At this stage, blood sugar management is your most powerful tool. Keeping your glucose levels within a healthy range can slow the progression of retinal damage and, in some cases, prevent the disease from advancing to a more serious stage. Blood pressure and cholesterol management also matter, as both conditions can accelerate damage to the retinal blood vessels.
At South Texas Eye Institute, Dr. Marten draws on her background in nutrition to educate patients on lifestyle and dietary choices that support better blood sugar control. This proactive, patient-centered approach helps you take an active role in protecting your vision long before advanced treatments become necessary.
Advanced Diabetic Retinopathy Treatment
When the condition progresses to proliferative diabetic retinopathy or when diabetic macular edema threatens central vision, your eye doctor may recommend one or more of the following treatments:
Anti-VEGF Eye Injections
Anti-VEGF (vascular endothelial growth factor) medications work by blocking a protein that signals the eye to grow abnormal new blood vessels. By slowing this growth, these injections also help reduce fluid buildup in the retina.
During the procedure, your eye doctor numbs the eye with topical anesthesia and then injects the medication directly into the vitreous. While the idea of an eye injection can feel intimidating, most patients report only mild, brief discomfort. These injections are typically repeated over multiple visits, and your eye doctor will monitor your response to determine the best ongoing schedule.
Laser Therapy (Photocoagulation)
Laser treatment uses focused beams of light to address damaged blood vessels in the retina. Focal laser photocoagulation targets specific leaking vessels and is commonly used to treat diabetic macular edema. The laser seals off the leaking areas, helping to reduce swelling and stabilize vision.
For proliferative diabetic retinopathy, a more extensive approach called scatter (pan-retinal) photocoagulation may be recommended. This technique applies laser burns across a wider area of the retina, which helps shrink abnormal blood vessels and discourage new ones from forming.
Laser therapy is usually performed in an office setting, and you may need more than one session. Some patients notice temporary blurriness for about a day afterward, and minor changes in peripheral or night vision may occur.
Vitrectomy Surgery
In cases where severe bleeding has clouded the vitreous or where scar tissue has caused retinal detachment, a surgical procedure called vitrectomy may be needed. During a vitrectomy, your eye surgeon makes small incisions in the white of the eye and uses specialized instruments to remove blood and scar tissue from inside the eye.
Vitrectomy is performed in a surgery center or hospital under local or general anesthesia. Recovery times vary, but many patients see gradual improvement in vision as the eye heals. Your eye doctor will provide specific post-operative instructions and schedule follow-up visits to monitor your progress.
Your Vision Is Worth Protecting
Diabetic retinopathy is a serious condition, but it does not have to mean losing your sight. With consistent diabetes management, regular dilated eye exams, and timely diabetic retinopathy treatment, you can take meaningful steps to preserve your vision for years to come.
Schedule a diabetic eye exam at South Texas Eye Institute in San Antonio, TX, to learn more about your treatment options and take the next step toward protecting your vision.


